After effective surgery, radiotherapy or chemotherapy, the biggest issue for cancer patients is recurrence, which is something almost every cancer patient would have. This is the same case for me.
There are two forms of cancer recurrence. The first one refers to the tumor recurring on the original foci, the second one refers to new tumor appearing at the new sites, which is called metastasis. Metastasis is the main reason of treatment failure and patient death. Cancer metastasis is generally considered to be a late-stage incident. However the latest research suggests that early-stage cancer could also have metastasis, manifesting in the blood and bone marrow. It is quite difficult for us to detect these cancer cells. The key to prevent recurrence is to eliminate the “metastasis” as early as possible, which means to destroy cancer cells in the blood and bone marrow.
Even though some cancer patients have undergone radical surgery clinically, postoperative chemotherapy is still given, what is called “neo-adjuvant chemotherapy”. The purpose is to eliminate cancer cells in the blood or bone marrow. It is commonly used for postoperative breast cancer, colorectal cancer and non-small cell lung cancer. However, many patients will still relapse after surgery. For example, the recurrence rate of stage two breast cancer is 30% within 5 years. A few patients will relapse after 20 years; the recurrence rate of stage two lung cancer reached as high as 60% within five years.
Chemotherapy cannot completely clear cancer cells. Firstly, some cancer cells are naturally are not sensitive to chemotherapy. Secondly, there are two kinds of cancer cells, the first one is the common type that is sensitive to chemotherapy, the second one is a stem cell type (cancer stem cells). So far neither chemotherapy (conventional dose) nor radiotherapy works on cancer stem cells. Moreover, conventional cancer cells, stimulated by chemotherapeutic drugs, could become genomically unstable developing into cancer stem cells.
Currently, it’s considered impossible for chemotherapy to eliminate all cancer cells, the last cancer cell in vivo can only be
cleared by immune cells.
I started to receive immunotherapy one week after surgery, including DC cellular immunity, CIK reinfusion, a combined vaccination, as well as regular injections of cytokines to date.
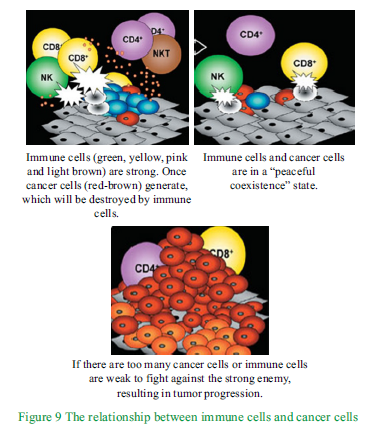
The cancer cells in the blood and bone marrow may not cause havoc for a long time. This is because there are immune cells in our bodies, such as T lymphocytes, Natural Killer cells (NK), which act like body guards, resisting and eliminating invading enemies (bacteria, viruses) and “traitors” evolving from normal cells, such as cancer cells. Immune cells keep watch on cells in the body, once there are cells “betraying” and developing into “bad cells” (atypical hyperplasia cells) or even “enemies” (cancer cells), immune cells would immediately “eat” and “surround” them to avoid harm to our human bodies, which is referred to as immune elimination. Sometimes there are many cancer cells which are forceful enough that immune cells can not destroy them, so the two sides are evenly matched in
strength. The cancer cells and immune cells are in a “peaceful coexistence” state, called “immune balance”. If there are too many cancer cells or immune cells are too weak to fight against a stronger enemy, cancer cells can escape from immune cells’ surveillance and grow rapidly, which is referred to as “immune escape.” Cancer metastasis occurs in the last case (see Figure 9).
In order to prevent cancer recurrence, we must protect the immune function. The immune system is complex, the immune cell compositions that work on cancer cells include (1) cytokines, such as interleukin (2) tumor necrosis factor, thymosin and interferon, etc. These factors are secreted by immune cells. Clinical cytokines are made through gene recombination technique; (2) immune cells, including lymphokine-activated killer cells (LAK), cytokine-induced killer cells (CIK) (mostly are NK cells), dendritic cells (DC) and T cells (CD4 and CD8 cells). These cells are interdependent and synergistic. Cytokine-induced killer cells and T cells can directly or indirectly kill cancer cells by secreting cytokines; dendritic cells can not directly kill cancer cells because they act as an intelligence cell. Cancer cells are very cunning, although
they have become traitors, their appearances almost mirror normal cells. Furthermore, cancer cells often disguise themselves with a coat composed of a special protein and in doing so become unrecognizable to CIK or T cells. Dendritic cells (DC) act like spies in our bodies and are especially there for collecting information like the intelligence of cancer cells, transferring this information to T cells and other immune cells to destroy cancer cells.
Cytokines (mainly interleukin-2) and immune cells (mainly LAK cells) have been applied in cancer treatment as early as the 1980s. Goldberg, a surgeon in the American National Cancer Institute isolated patient’s own peripheral blood mononuclear cells, and then cultured these cells with interleukin-2 in vitro laboratory, with the aim of increasing the number of cells and improving cell activity. Finally these cells could be reinjected into the patient, this is referred to as LAK therapy. By 1985, he had treated 25 patients with advanced cancer using this method, 11 patients experienced tumor shrinkage and a malignant melanoma patient’s tumors disappeared for 10 months. In 1987, Rosenberg and his research group also reported that this therapy was most effective for renal cancer, melanoma and colorectal cancer according to the results of 157 cases.
Rosenberg’s cancer therapy excited people for a period of time, but it ended too soon, mainly because (1) it failed to prove that this treatment can prolong patient’s lives; (2) the therapy was very complicated because the cell separator needs to be applied to isolate mononuclear cells, this carries certain risks to patients; (3) large doses of interleukin-2 needed to be used which almost every patient would have side effects towards, the most serious ones would be pulmonary edema, hypotension and renal dysfunction.
During the years 1993-1995, I applied modified LAK therapy to treat more than thirty patients with advanced cancer. There was a 67 year-old esophageal cancer patient Mr. Chen who came from Shenzhen, experiencing dysphagia for two months. I performed an endoscopy for him and found an eight-centimeter esophageal stenosis on the lower esophagus with an uneven surface, which a biopsy proved to be squamous cell carcinoma. The patient had heart disease and refused surgery, consequently I preformed LAK therapy on him. One month later his condition improved markedly. But we had lost contact with each other in recent years. Last year, his daughter came to look for me in Guangzhou because of another member of her family with cancer. She told me that her father died of a heart attack three years ago however his esophageal cancer did not relapse. He received cancer treatment in 1994 and died in 2007. That is to say, no matter which kind of disease he died of, he had survived for a full 13 years after he suffered from cancer, which could be considered a miracle.
From the end of the last century to the beginning of this century, immunotherapy has mostly remained in the theoretical research stage. There was rare international literature concerning immunotherapy and the possibility that it could really prolong survival time or even cure diseases. An article published in the “New England Journal of Medicine” in 2008 renewed the public’s interest in cancer immunotherapy(Figure 10), the authors were Dr. Yee and Dr. Hunder from the Fred Hutchinson Cancer Research Centre in Seattle, America. They reported on a 52-year-old male patient who suffered from recurrent melanoma with right lung, pleura, left iliac fossa and inguinal
metastases. He had undergone chemotherapy, high-dose interleukin-2 and interferon therapy, which were all noneffective. They isolated the patient's peripheral blood mononuclear cells by a cell separator. Dendritic cells isolated from peripheral blood were stimulated by a special melanoma antigen and cultured with T cells, then using a specific antigen to stimulate T cells. By repeated cell culture, purification
(clone) and amplification till the 18th day, T cells were reinjected into the body through the veins. Totally 5 billion cells were reinjected within two hours. Three days after re infusion, the patient only had a light fever and weakness. Two months later, the patient had a PET-CT scan and CT scan, the metastatic lesions in lung and pelvic cavity had disappeared. By the time the authors reported this article, the patient was disease-free and survived for twenty-six months.

This article was published in one of the world's most authoritative medical journals, they reported the patient’s case in six pages, which could be regarded as very rare. Why was this article so highly valued? It is mainly because melanoma is most common in Caucasians. Once there is a metastasis, patient’s survival time is very short. According to reports in the US, if patients with stage IV melanoma have one metastasis, the median survival time will be seven months; if there are two parts of metastases, the median survival time will be four
months; while if there are three metastases, the median survival time will only be two months; if there are visceral organ metastases such as lung metastasis, the prognosis would be worse, the survival time is generally only three months. The patient reported on this article had three or more parts of metastases, he was then disease-free and survived of more than 2 years after CD4 T cells treatment, which was certainly a remarkable achievement. This fact indicates that immunotherapy can cure cancer.