Hyperthermic intraperitoneal chemotherapy (HIPEC) or Intraperitoneal hyperthermic chemoperfusion (IPHC) is a type of hyperthermia therapy in combination with surgery in the treatment of advanced abdominal cancers. In this procedure, warmed anti-cancer drugs are infused and circulated in the peritoneal cavity (abdomen) for a short period of time to prevent and treat implantation metastasis of abdominal malignant tumors.
Unlike systemic chemotherapy delivery, which circulates throughout the body via the bloodstream, HIPEC delivers chemotherapy directly to cancer cells in the abdomen. This allows for higher doses of chemotherapy treatment. Heating the solution may also improve the absorption of chemotherapy drugs by tumors and destroy microscopic cancer cells that remain in the abdomen after surgery.
Before patients receive HIPEC treatment, doctors perform cytoreductive surgery—a procedure to debulk, or reduce, the size of a cancerous tumor—within the abdomen. When as many tumors as possible have been removed, a heated, sterilized chemotherapy solution is delivered to the abdomen to penetrate and destroy remaining cancer cells. The solution is 41 to 42 degrees Celsius, about the temperature of a warm bath. It is circulated throughout the abdomen for approximately 90 minutes. The solution is then drained from the abdomen, and the incision is closed.
Principles
1. Heating can destroy the balance of cell membrane so that molecule can easily go through the membrane. Hyperthermia works with chemotherapeutic drugs to fight against tumor, and the effect will be significantly enhanced when the temperature reaches 43℃. The heat effect can raise permeability of anticancer drugs from depth of 1-2mm to 5mm.
2. There is difference of heat tolerance between tumor cells and normal cells. Normal cells can tolerate the heat of 45℃ while tumor cells will be destroyed in the heat of 40-43℃. In this case, tumor cells will be killed while normal cells unharmed.
3. Continuous circulatory perfusion has a mechanical scouring effect on free cancer cells and small peritoneal metastatic lesions in the abdominal cavity, which can induce anoikis or directly lead to the death of the tumor (apoptosis under special circumstances outside the original living environment), so as to clear the remaining cancer cells and small metastatic lesions in the abdominal cavity.
4. Effective drug delivery inside the abdominal cavity, partial in large volume and high concentration of chemotherapeutic drugs, make the intraperitoneal free cancer cells and postoperative residual microscopic carcinoma directly immerse in a high concentration of chemotherapy medicine. Peritoneal barrier will slow down drug metabolism, and keep high drug concentrations for a long time (cisplatin: abdominal drug concentration is 73 times of that in plasma; 65% of cisplatin remains in the body after drainage of abdominal fluid), effectively killing tumor cells and reducing or avoiding the systemic side effects.
During HIPEC, either single administration or combined sequential administration can be performed. At present, there is no unified standard for the dose of chemotherapeutic drugs. If combined with intravenous administration, the dose should be reduced.
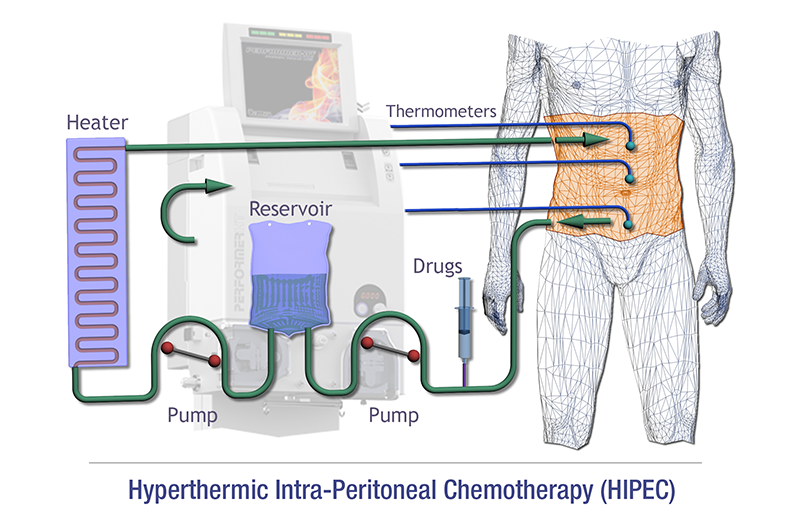
Uses of HIPEC
IPHC is generally used after surgical removal of as much cancer as possible (debulking), which may include the removal of all involved peritoneal areas. IPHC is used as a viable solution for certain advanced stage tumors in the abdomen that have spread many small tumors throughout the abdomen, when surgery is not likely to be possible or effective. It can also be applied, during surgery, directly on the area, for those whose abdominal cancer is advanced but is still considered surgically resectable, as an alternative to surgery and traditional chemotherapy alone.
The diseases most often treated with this method are cancer of the appendix, colorectal cancer, ovarian cancer, desmoplastic small round cell tumor, gastric cancer, mucinous adenocarcinoma of appendix, mesothelioma, low-grade sarcoma.
Advantage
HIPEC is a prevention and treatment measure of abdominal malignant tumors, especially peritoneal recurrence of postoperative gastrointestinal cancer and liver metastasis. With the combination of local chemotherapy and hyperthermia, a large amount of chemotherapeutic drug fluid flushing in abdominal cavity boasts the effect of pharmacokinetics and fluid dynamics, effectively removing free cancer cells and tiny cancer lesions, preventing postoperative abdominal recurrence and liver metastasis and improving the survival rate and quality of life. HIPEC is a safe, convenient and practical procedure with fewer side effects and fewer complications, and it can be used for several times. It is a reasonable surgical adjuvant treatment for abdominal malignant tumors. At the same time, it is also one of the best treatments for malignant ascites and an indispensable method for treating abdominal tumors.
Indication
HIPEC has a unique effect on the prevention and treatment of malignant ascites and peritoneal implantation metastasis of malignant tumors such as gastric cancer, colorectal cancer, ovarian cancer, appendiceal cancer, low grade sarcoma, peritoneal pseudomyxoma, peritoneal malignant mesothelioma, liver cancer, bile duct cancer and pancreatic cancer.
Contraindication
(1) Extensive adhesion in the abdominal cavity caused by various reasons;
(2) Patients with bad healing factors such as edema, ischemia and tension at the anastomotic site;
(3) Patients with intestinal obstruction;
(4) Patients with obvious hepatic and renal insufficiency;
(5) Severe cardiovascular diseases;
(6) Unstable vital signs;
(7) Cachexia patients.